Sacral Nerve Compression
What is Sacral Nerve Compression?
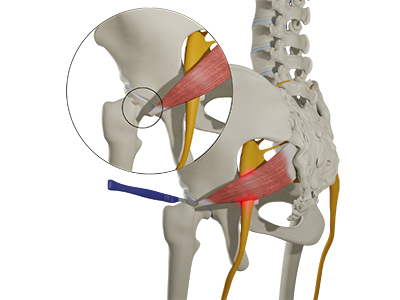
Sacral nerve compression refers to pressure or irritation of the sacral nerves, which are a group of nerves emerging from the lower part of the spine (sacrum) that control sensation and movement in the pelvis, legs, and lower back. This compression can interfere with nerve function and cause a variety of symptoms depending on the specific nerves affected.
What are the Causes of Sacral Nerve Compression?
Causes of sacral nerve compression include:
- Herniated Disc: Bulging or ruptured spinal disc pressing on sacral nerves.
- Spinal Stenosis: Narrowing of the spinal canal in the lower spine.
- Trauma or Fractures: Injury to the sacrum affecting nearby nerves.
- Tumors or Cysts: Growths that apply pressure on sacral nerve roots.
- Degenerative Disc Disease: Wear and tear that alters spinal structure and pinches nerves.
- Infections or Abscesses: Inflammatory processes compressing the nerves.
- Scar Tissue (Post-surgery): Adhesions pressing on the nerves after spine surgery.
What are the Symptoms of Sacral Nerve Compression?
Symptoms of sacral nerve compression may include:
- Lower back or pelvic pain
- Radiating pain to the buttocks, hips, or legs
- Numbness or tingling in the legs or feet
- Muscle weakness in the lower limbs
- Difficulty walking or standing for long periods
- Bladder or bowel dysfunction (in severe cases)
- Sexual dysfunction in some individuals
How is Sacral Nerve Compression Diagnosed?
Sacral nerve compression is diagnosed through a combination of:
- Medical history and physical examination to assess symptoms and nerve function
- Neurological tests to check muscle strength, reflexes, and sensation
- Imaging studies such as MRI or CT scans to visualize nerve compression
- Electromyography (EMG) and nerve conduction studies to evaluate nerve activity and damage
How is Sacral Nerve Compression Treated?
Sacral nerve compression treatment depends on the cause, severity of symptoms, and whether there’s nerve damage. The goal is to relieve pressure on the nerve, reduce pain, and restore function. Treatment typically begins conservatively and progresses to surgery if needed. These include:
Non-Surgical Treatments
- Medications: These include NSAIDs, such as ibuprofen and naproxen, to reduce inflammation and pain, muscle relaxants for associated muscle spasms, and neuropathic agents such as gabapentin and pregabalin for nerve pain.
- Physical Therapy: This involves exercises to improve flexibility, strength, and spinal alignment, posture correction and core strengthening, and pelvic floor therapy if bladder or bowel symptoms are present.
- Epidural Steroid Injections: Corticosteroids are injected around the sacral nerves to reduce inflammation and pain. This is often used when pain is severe and not relieved by oral medications.
- Lifestyle Modifications: This involves measures such as avoiding prolonged sitting or heavy lifting, weight loss if overweight, and ergonomic adjustments in daily activities.
- Assistive Devices: Use of braces or supports to stabilize the pelvis or spine during healing.
- Alternative Therapies (if appropriate): These include methods such as acupuncture, chiropractic care, and TENS (Transcutaneous Electrical Nerve Stimulation).
Surgical Treatments
Surgery may be needed if symptoms persist after conservative treatment, there is significant nerve compression or damage, and there are bladder or bowel control problems. Common surgical options include:
- Laminectomy or Discectomy: This procedure removes part of the bone or herniated disc pressing on the sacral nerve.
- Foraminotomy: This procedure widens the foramen (nerve exit point) to relieve pressure.
- Sacral Nerve Stimulation: This is a therapy that uses a small implanted device to deliver electrical impulses to the sacral nerves (used for bowel/bladder control issues).
- Tumor/Cyst Removal: This procedure involves removing growths, such as a Tarlov cyst that applies pressure on sacral nerve roots.