Thoracic Facet Radiofrequency Ablation
What is Thoracic Facet Radiofrequency Ablation?
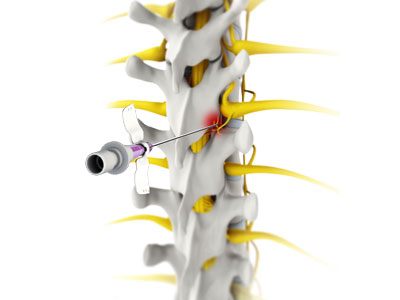
Thoracic Facet Radiofrequency Ablation (RFA) is a minimally invasive pain management procedure designed to provide long-term relief from chronic thoracic spine pain arising from the facet joints. These joints, located between the vertebrae, can become a source of pain due to arthritis, injury, or mechanical stress. RFA targets the medial branch nerves that transmit pain signals from the affected facet joints to the brain.
Indications for Thoracic Facet Radiofrequency Ablation
Thoracic Facet RFA is primarily indicated for:
- Chronic mid-back pain originating from the thoracic facet joints.
- Pain unresponsive to conservative management, such as medications, physiotherapy, or injections.
- Confirmed diagnosis of thoracic facet-mediated pain through diagnostic medial branch nerve blocks.
- Degenerative joint disease, postural strain, or minor trauma-related thoracic pain.
Contraindications for Thoracic Facet Radiofrequency Ablation
Thoracic Facet RFA is not indicated in cases of:
- Local infection at the insertion site.
- Coagulopathy or bleeding disorders.
- Uncontrolled diabetes or severe systemic illness.
- Pregnancy (relative contraindication).
- Inability to tolerate the prone position.
Procedure for Thoracic Facet Radiofrequency Ablation
Thoracic Facet RFA procedure involves following steps:
- Preparation: You will be placed in a prone position, and the thoracic area is sterilized. Local anesthesia is administered at the targeted levels.
- Imaging Guidance: Fluoroscopy (X-ray guidance) is used to accurately identify the thoracic facet joints and guide the placement of the radiofrequency needle.
- Needle Placement: A specialized radiofrequency needle is advanced near the medial branch nerve of the targeted thoracic facet joint. Sensory and motor stimulation tests confirm the correct placement.
- Ablation: After confirmation, the tip of the needle is heated (usually to 80–90°C) for 60–90 seconds. The thermal lesion disrupts the pain-transmitting medial branch nerve, preventing it from sending pain signals.
- Completion: The needle is removed, and a sterile dressing is applied. You are monitored briefly before discharge.
How does Thoracic Facet Radiofrequency Ablation Work to Control Pain?
During RFA, controlled thermal energy is applied to the medial branch nerves that supply the facet joints. This heat denatures the nerve proteins, resulting in interruption of pain transmission pathways without affecting motor function or spinal stability. Over time, these nerves may regenerate, but pain relief can last for several months to years.
Post-Procedure Care for Thoracic Facet Radiofrequency Ablation
After thoracic facet RFA procedure, post care involves:
- Rest for 24 hours following the procedure.
- Gradual return to normal activity.
- Application of ice packs to reduce soreness.
- Follow-up visit to assess pain relief and functional improvement.
- Physical therapy may be recommended to strengthen supporting muscles.
Complications of Thoracic Facet Radiofrequency Ablation
Though rare, possible complications of thoracic facet RFA include:
- Temporary localized pain or numbness.
- Bleeding or infection at the injection site.
- Nerve injury (extremely uncommon).
- Allergic reaction to medications or contrast dye.
Outcomes of Thoracic Facet Radiofrequency Ablation
Most individuals experience significant pain reduction within 1–3 weeks following the procedure. Pain relief typically lasts 6 to 18 months, depending on individual healing and nerve regeneration rates. Repeat ablation may be performed if pain recurs.